Bailey Klingaman explores the history of intravenous infusion therapy and the path to modern treatments. Deb DiTrapano, MSN, RN, OCN predicts the implementation of artificial intelligence in infusion therapy and discusses the effects of the nurse shortage.

In the 600 years since infusion therapy was first documented, there have been countless experiments, lives saved and lost, and great innovations made to improve the treatment for patients and clinicians. However, our current methods and devices are not fool-proof, and we still make efforts today to prioritize safety and efficiency for the practice of intravenous infusion.
A Brief History of IV Therapy
The first documented instance of infusion therapy can be traced back to 1492, when a doctor attempted a blood transfusion between three young boys and Pope Innocent VIII. The unsuccessful attempt was the first of many infusion experiments to come, although there is no further documentation for over 150 years.
In 1658, Sir Christopher Wren completed the first successful IV device using a pig’s bladder and quill to infuse a liquid mixture into the veins of a dog. Over the next 200 years, doctors would investigate animal-to-human transfusions, human-to-human transfusions, and the durability of different IV devices.
It wasn’t until the 1940s that nurses were allowed to administer infusions – a task formerly reserved for doctors – in order to enhance the speed of treatment for those injured during WWII. In the 1950s, intravenous therapy became a widely used practice in hospitals, and the plastic infusion bag was introduced.
Since then, we have seen the development of ambulatory infusion pumps, electromechanical pumps, and volumetric pumps. Intravenous therapy has been recognized as a method for blood transfusions, administering nutrients, and injecting medical solutions into the veins.
IV Therapy in Today’s World
It is undeniable that healthcare has come a long way in the last few decades, let alone the century. With the advancement of technology and the introduction of creations like vein-finder technology, barcode scanners, smart pumps, and healthcare information technology, infusion therapy is safer and more efficient than ever before.
With that being said, it is important to acknowledge the current causes of errors so that we can improve our modern technologies and reduce the risks.
Top Causes of Medication Errors:
- Lack of knowledge about the drug
- Miscalculations
- Failure to double-check procedures
- Confusion between look-alike, sound-alike medications
- Inappropriate dosage
- Multi-drug interactions
- Lack of drug indication data
- Distractions and interruptions
- Overburdened healthcare systems
Despite the risks that seem around every corner, technology helps us significantly in counteracting many of the causes of errors. Task automation, medical alerts, reporting features, information sharing, computer-assisted communication, and the standardization of practices are only some of the capabilities of today’s systems.
Vein-Finder Technology
The nursing skill required to successfully start a peripheral IV requires extensive knowledge and practice. To advance from novice to expert takes years of nursing experience and a thorough understanding of infusion therapy competency and complications. In recent years, learning the skill of vein selection has been made easier with the use of FDA-approved near-infrared (NIR) superficial vein imaging technology.
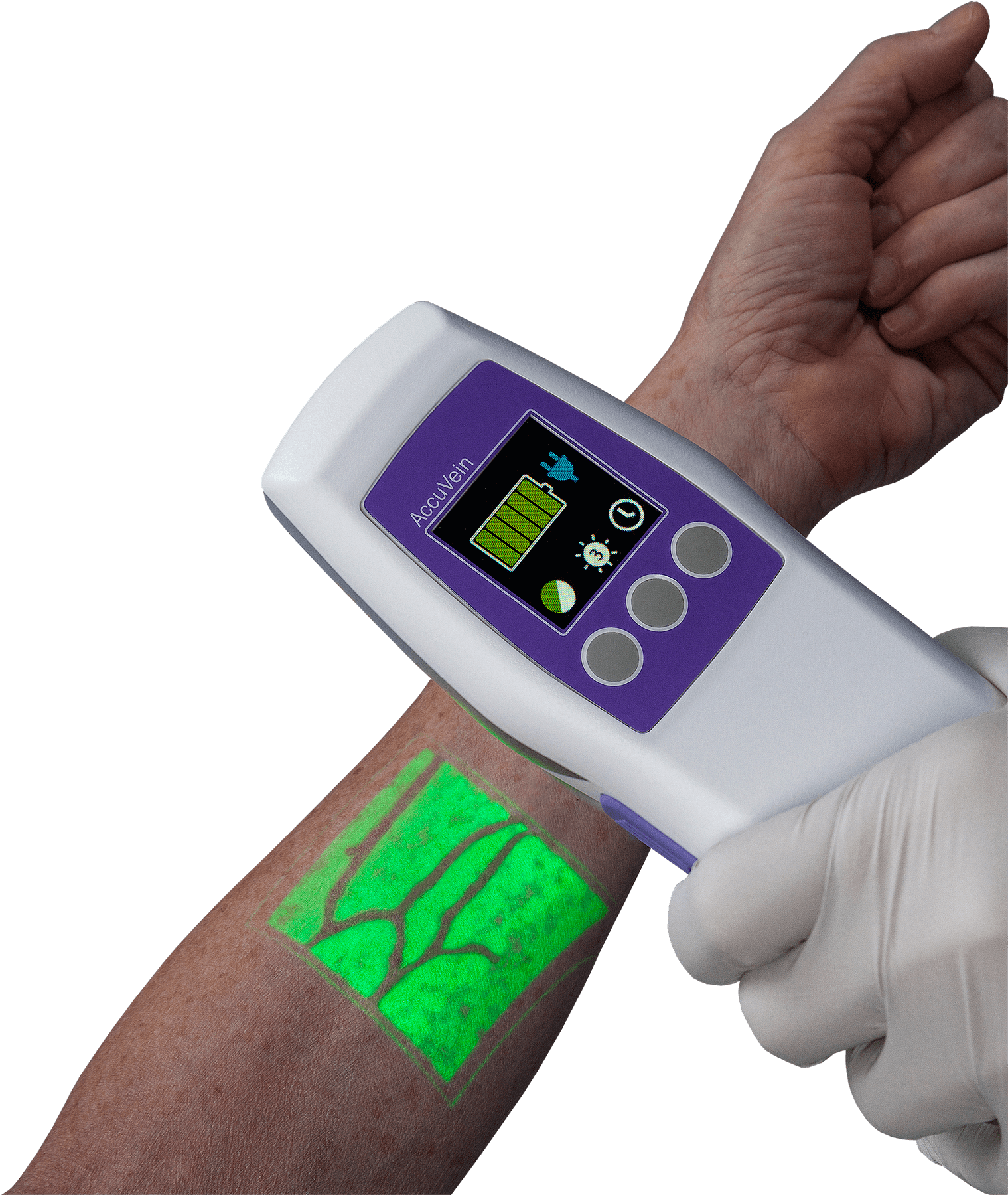
Companies like AccuVein have designed NIR imaging technology that illuminates the veins of a patient, showing the clinician several possible destinations of successful peripheral IV insertion. Vein-finder technology is particularly helpful when used with “difficult sticks”; patients whose veins easily collapse, roll, are too thin, or are difficult to find. Proficiency in using a vein finder assures an increased level of comfort, and is proven to increase confidence for nurses and patients alike.
Clinicians can also use the adult difficulty IV access (A-DIVA) score, a tool that helps identify difficult stick patients by calculating a prediction for the failed first attempt rate, which is 37% for 2-3 points and 94% for 4-5 points. Calculate the score by adding one point for each of the following criteria met:
- Known history of difficult IV access
- Expect failed first attempt or difficult IV access
- Inability to identify a dilated vein by palpating the upper extremity (after tourniquet placement)
- Inability to identify a vein by visualizing the upper extremity (after tourniquet placement)
- The largest dilated vein has a diameter <3 mm (after tourniquet placement)
Barcode Scanners
 According to a study conducted by the National Library of Medicine, the use of barcode administration systems and scanners reduces the number of adverse drug events and contributes up to an 80% reduction in administration errors.
According to a study conducted by the National Library of Medicine, the use of barcode administration systems and scanners reduces the number of adverse drug events and contributes up to an 80% reduction in administration errors.
Manufacturing companies like Zebra Technologies have developed barcode scanners that have full-fleet remote management, device health visibility, and high scanning accuracy on a variety of surfaces. These scanners are made to last for an entire shift to ensure uninterrupted care and the elimination of scanning-related distractions.
Implementing barcode systems works to ensure the right patient receives the correct medication, a solution to the confusion between look-alike, sound-alike medications, and any possible drug mix-ups.
Infusion Pumps
The average modern infusion pump is designed to incorporate patient identification, weight, and height. Clinicians can often enter the patient’s medication allergies, which can be identified by the pump and generate an alert if the patient is at risk. Smart infusion pumps take error prevention even further. These pumps alert clinicians if the infusion rate is outside of the safety limits, reducing the risk of calculation errors.
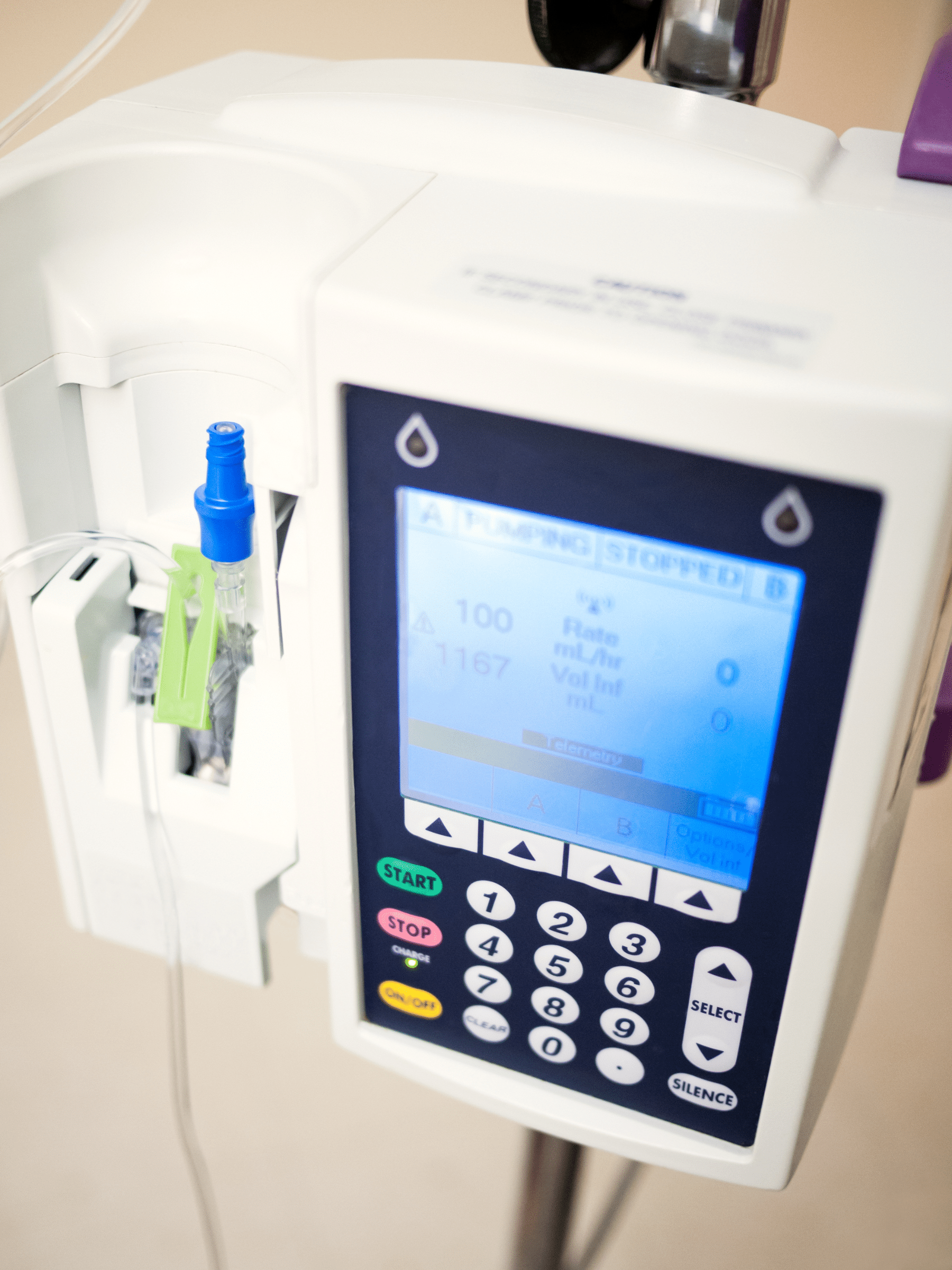 Zyno Medical designs and manufactures infusion pumps with multi-therapy programming in mind. With set-based and pump-based free flow protection, alarm modes, occlusion and air-in-line detection levels, and more, infusion pumps like these are built to increase efficiency and patient safety.
Zyno Medical designs and manufactures infusion pumps with multi-therapy programming in mind. With set-based and pump-based free flow protection, alarm modes, occlusion and air-in-line detection levels, and more, infusion pumps like these are built to increase efficiency and patient safety.
Eitan Medical is another creator of great infusion pumps. Eitan’s compact and lightweight Sapphire pumps have touch-screen interfaces, authorization levels, indications of infusion parameters, and more. These pumps were designed with patient safety and error prevention in mind.
Utilizing infusion pumps that have the ability to make calculations, alert the clinician about patient allergies, and flag potential risks actively counteracts miscalculations, inappropriate dosages, and possible drug interactions not caught by the prescriber. However, this is with the expectation that the infusion practice is keeping updated records of the drug information and instructions.
Healthcare Information Technology
Healthcare information technology (HIT) is “the storage, retrieval, sharing, and use of healthcare information, data, and knowledge for communication and decision making” that incorporates computer hardware and software. These solutions reduce the chance of human error, improves efficiency, tracks and stores data, and more. Different HITs have different purposes, but have generally improved the clinical outcomes of the practice and increased patient safety.
For example, RxToolKit is a software solution that eliminates the potential for using outdated medication guides or package inserts, has drug-specific calculators, and ensures cohesive training for all clinicians in the infusion practice. RxToolKit’s team of clinicians creates condensed infusion medication guides detailing drug information, indications and contraindications, warnings, use in specific populations, and patient resources. Based on these drug monographs, comprehensive courses and assessments are created to train clinicians and report competence results to clinical managers.
WeInfuse is another infusion software solution created to improve outcomes and increase efficiency. As an end-to-end SaaS solution, WeInfuse streamlines the infusion workflow, featuring patient and order management; scheduling; inventory management; billing and claims; reporting and analytics, and more. The software has been proven to increase profitability for infusion centers and pharmacies.
The Future of Infusions
By now, we’ve explored the past and present solutions to infusion therapy safety risks and how we have overcome many of the challenges. Still, we must recognize that like all healthcare fields, the practice of infusion is complicated and risks to safety remain.
- In 2020, there were 500,000 estimated medication errors per day in the United States.
- The United States spends approximately $21 billion each year in response to preventable medication errors.
- There are 21 possible instances of an error in the process of completing a single infusion.

Human error is the common denominator associated with many of the top causes of medication errors. As we look to the future of infusion therapy, we must consider safety as our number one priority. But how can we decrease the potential safety risks due to human error?
The basis of safe healthcare practices relies on:
- Evidence-based practices
- Standardized processes and procedures
- Education and competency
- Consistent compliance to standards
The Nurse Shortage
While there have been great advances in healthcare through the decades, the supply of competent providers has not kept pace with the ongoing demand. Shortages are at an all-time high post-COVID, as many experienced nursing staff have left their positions due to the extreme working conditions during the pandemic. With mid-50s as the average age of nurses, retirement is on the horizon for many more clinicians.
The question is, how do we provide the safest care to patients while recruiting and retaining the younger workforce into the profession? Sheer determination will not get us where we need to go, but by embracing existing technology and encouraging the implementation of new ideas, we may be able to fix the shortage.
Artificial Intelligence in Healthcare
Artificial intelligence (AI) is a key ingredient to the future of safer, more efficient infusion therapy. Tools that enhance nursing skills, increase competence and confidence in nurses, and have the availability to access accurate information streamline the process of safe care delivery.
Utilizing AI in the healthcare setting has proven to reduce costs, increase efficiency, and improve staff and patient experiences. With the correct implementation, this technology can assist rather than threaten the workforce. For example, using self-service kiosks for check-in ensures staff are able to answer clinical questions, pursue a clinical position if not already held, and provide better infusion care.
The Possibilities
While technology isn’t foolproof–and AI technology is no exception–it has done much to enhance infusion care outcomes and patient safety. From animal-to-human transfusions to error-preventative infusion pumps, administering infusions is safer than ever before.
- While there have been many advancements in the infusion practice, there are issues that have yet to be addressed. But with each problem that arises, so does the opportunity for improvement. With all of these possibilities, the future of IV therapy is promising.
References:
Alotaibi, Y. K., & Federico, F. (2017, December). The Impact of Health Information Technology on Patient Safety. Saudi Medical Journal. Retrieved February 23, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5787626/
Artificial Intelligence in Healthcare: Benefits and challenges of Machine Learning Technologies for Medical Diagnostics. U.S. Government Accountability Office. (2022, November 10). Retrieved March 10, 2023, from https://www.gao.gov/products/gao-22-104629
A brief history of IV infusion therapy, from the Middle Ages to today. Med One Group. (2018, January 17). Retrieved February 20, 2023, from https://www.medonegroup.com/aboutus/blog/a-brief-history-of-iv-infusion-therapy
Barth, S. (n.d.). Artificial Intelligence (AI) in Healthcare & Hospitals. ForeSee Medical. Retrieved March 10, 2023, from https://www.foreseemed.com/artificial-intelligence-in-healthcare
Benner, P., Tanner, C. A., & Chesla, C. A. (2009). Expertise in Nursing Practice: Caring, Clinical Judgement, and Ethics (2nd ed.). Springer Publishing Company.
Ehdadmin. (2022, February 19). The history & development of intravenous therapy – IV boost UK. IVBoost. Retrieved February 20, 2023, from https://ivboost.uk/history-development-intravenous-therapy/
Frank, R. L. (2023, January 19). Peripheral venous access in adults. UpToDate. Retrieved March 20, 2023, from https://www.uptodate.com/contents/peripheral-venous-access-in-adults?search=difficult+peripheral+venous+access+in+adults &%3Bsource=search_result&%3BselectedTitle=1~150&%3Busage_type=default&%3Bdisplay_rank=1
Journal of Nursing Regulation. (n.d.). National Nursing Workforce Study. NCSBN. Retrieved March 20, 2023, from https://www.ncsbn.org/research/recent-research/workforce.page
Kiel, PhD, J. M., & Linkov, MPH, PhD, F. (2022, July 11). The role of artificial intelligence in enhancing the delivery of healthcare. Journal of AHIMA. Retrieved March 10, 2023, from https://journal.ahima.org/page/the-role-of-artificial-intelligence-in-enhancing-the-delivery-of-healthcare
Kriwet, C. (2020, January 7). Here are 3 ways AI will change healthcare by 2030. World Economic Forum. Retrieved March 10, 2023, from https://www.weforum.org/agenda/2020/01/future-of-artificial-intelligence-healthcare-delivery/
Kuitunen, S., Niittynen, I., Airaksinen, M., & Holmström, A.-R. (2021, December 1). Systemic causes of in-hospital intravenous medication errors: A systematic review. Journal of patient safety. Retrieved February 23, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8612891/#:~:text=Insufficient%20actions%20to%20secure%20safe,causes%2 0of%20intravenous%20medication%20errors
Leung, A. A., Denham, C. R., Gandhi, T. K., Bane, A., Churchill, W. W., Bates, D. W., & Poon, E. G. (2015, June). A Safe Practice Standard for Barcode Technology. Journal of patient safety. Retrieved February 23, 2023, from https://pubmed.ncbi.nlm.nih.gov/24618650/
Munro, C. L., & Hope, A. A. (2022, January 1). Improving Nurse Well-being: The Need Is Urgent and the Time Is Now. American Association of Colleges of Nursing. Retrieved March 20, 2023, from https://aacnjournals.org/ajcconline/article-standard/31/1/4/31651/Improving-Nurse-Well-being-The-Need-Is-Urgent-and
Rasool, M. F., Rehman, A. ur, Imran, I., Abbas, S., Shah, S., Abbas, G., Khan, I., Shakeel, S., Ahmad Hassali, M. A., & Hayat, K. (2020, October 13). Risk factors associated with medication errors among patients suffering from chronic disorders. Frontiers. Retrieved February 23, 2023, from https://www.frontiersin.org/articles/10.3389/fpubh.2020.531038/full
Rodziewicz, T. L., Houseman, B., & Hipskind, J. E. (n.d.). Medical error reduction and prevention. StatPearls. Retrieved February 23, 2023, from https://www.ncbi.nlm.nih.gov/books/NBK499956/
Schnelldorfer, T., Gurley, H., Errico, V. M., Price, L. M., Schwartz, J. J., Sahore, R., Cote, K., & Ruthazer, R. (2019, December 17). The Efficacy of Near-infrared Vein Imaging for the Success of Placing Peripheral Venous Catheters in Adults with Difficult Venous Access. Lahey Hospital and Medical Center.
Summa-Sorgini, C., Fernandes, V., Lubchansky, S., Mehta, S., Hallett, D., Bailie, T., Lapinsky, S. E., & Burry, L. (2012, January). Errors Associated with IV Infusions in Critical Care. The Canadian journal of hospital pharmacy. Retrieved February 23, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3282194/#
Team, S. C. (2023, February 4). Medication Errors Statistics. The Checkup. Retrieved February 23, 2023, from https://www.singlecare.com/blog/news/medication-errors-statistics/#
Truitt, E., Thompson, R., Blazey-Martin, D., NiSai, D., & Salem, D. (2016, June). Effect of the Implementation of Barcode Technology and an Electronic Medication Administration Record on Adverse Drug Events. Hospital Pharmacy. Retrieved February 23, 2023, from https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4911988/
Turner, N. (2013, November 2). The invention of IV fluid therapy. History of Nephrology. Retrieved February 20, 2023, from https://historyofnephrology.blogspot.com/2013/11/the-invention-of-iv-fluid-therapy.html
Weinstein, S. M. (2016, June 19). History of infusion therapy. Nurse Key. Retrieved February 20, 2023, from https://nursekey.com/history-of-infusion-therapy/
Yilmaz, H., Çinar Yücel, S., Ergin, E., Bagci, H., & Khorshid, L. (2021, October 22). Does the use of Infrared Technology (AccuVein AV-500®) for peripheral intravenous cannulation (PIVC) increase the success rate in nursing students? A randomized controlled trial. Nurse Education Today. Retrieved March 20, 2023, from https://www.sciencedirect.com/science/article/abs/pii/S0260691721004366?via%3Dihub




