Understanding proper medication administration, including the calculations necessary to safely administer drugs to patients, is a vital skill for all kinds of nurses and clinicians. Miscalculations are one of the three most common errors that occur in medication dispensing, and are largely preventable with the right comprehension, training, and tools.
For those considering becoming an infusion nurse or pharmacist, hear from experienced clinicians about why they chose to enter their professions and the kinds of responsibilities that can be expected in RxToolKit’s previous blog, “The Infusion Nurse & the Pharmacist”.
Particularly for clinicians in the infusion industry, where introducing medications into the vein or subcutaneous tissue is the primary objective, having a thorough comprehension of common IV calculations involved in the preparation and administration of intravenous drugs is paramount.
Common Abbreviations & Conversions
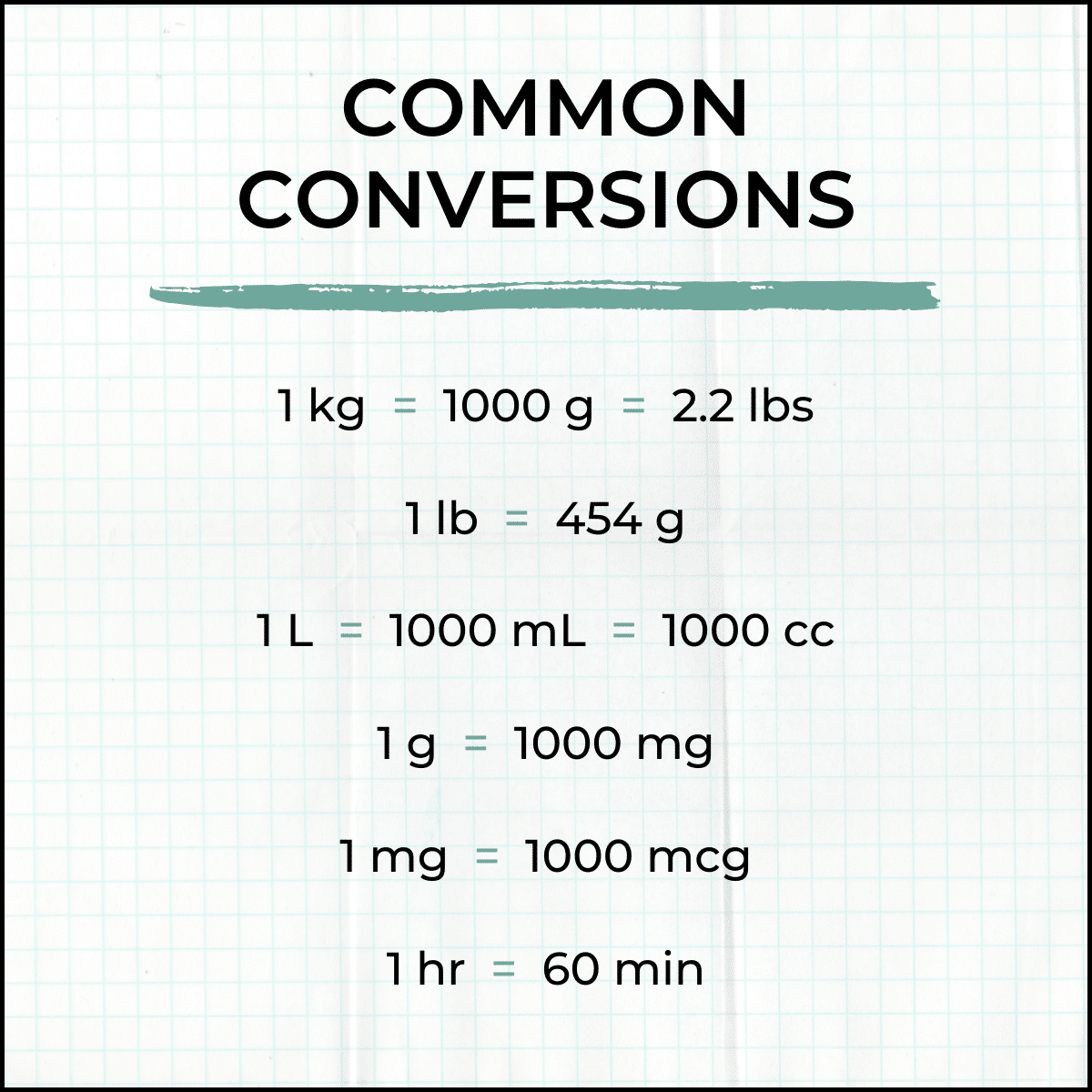
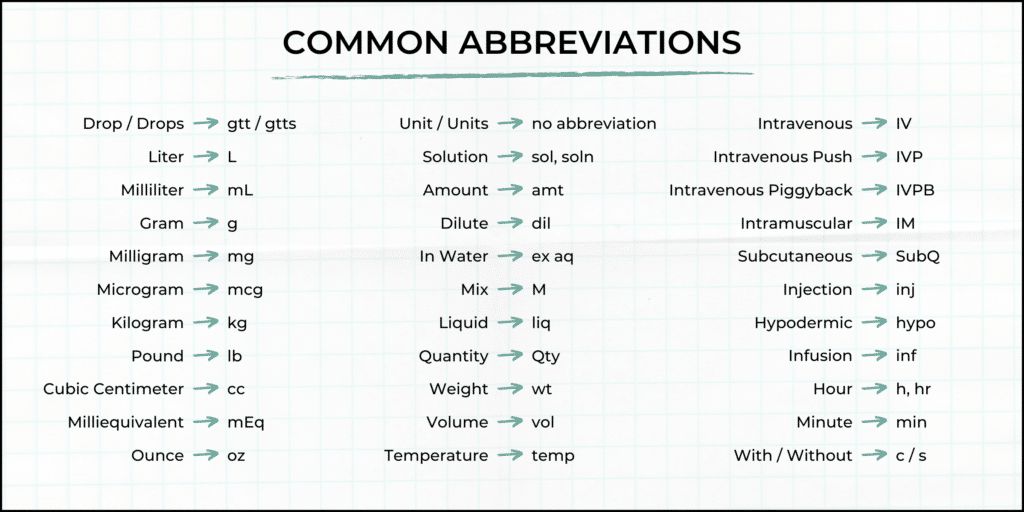
Some of the most frequent conversions seen in the infusion setting include metric conversions for measuring the volume, mass, and area of liquids. Many of these IV conversions utilize the official abbreviations for the units of measure, some of which are widely known outside of healthcare (e.g. minute:min, pound:lb) and others that are more niche terms (e.g. drop:gtt, milliequivalent:mEq).
It is important to familiarize yourself with these common abbreviations and conversions, as they can be seen often in the field and certain formulas may rely on your understanding.
IV Calculations & Definitions
In addition to understanding conversions and infusion-related abbreviations, anyone entering this industry should have a grasp of the primary terms involved in the IV calculations they will need to complete, as well as how to work out the math.
Drop/Gtt
Noted as a common abbreviation in infusion documentation, a drop (gtt) is a unit of measure used for continuous medication administration. It can help clinicians ensure that patients are receiving the correct amount of medication at an appropriate rate.
IV Drop Factor
The IV drop factor refers to the number of drops in 1 mL of a solution. This is a predetermined number that can be found on the IV tubing packages (i.e. microdrip and macrodrip tubing). Microdrip and macrodrip refer to the diameter of the needle where the drop enters the drip chamber, and both have specific purposes.
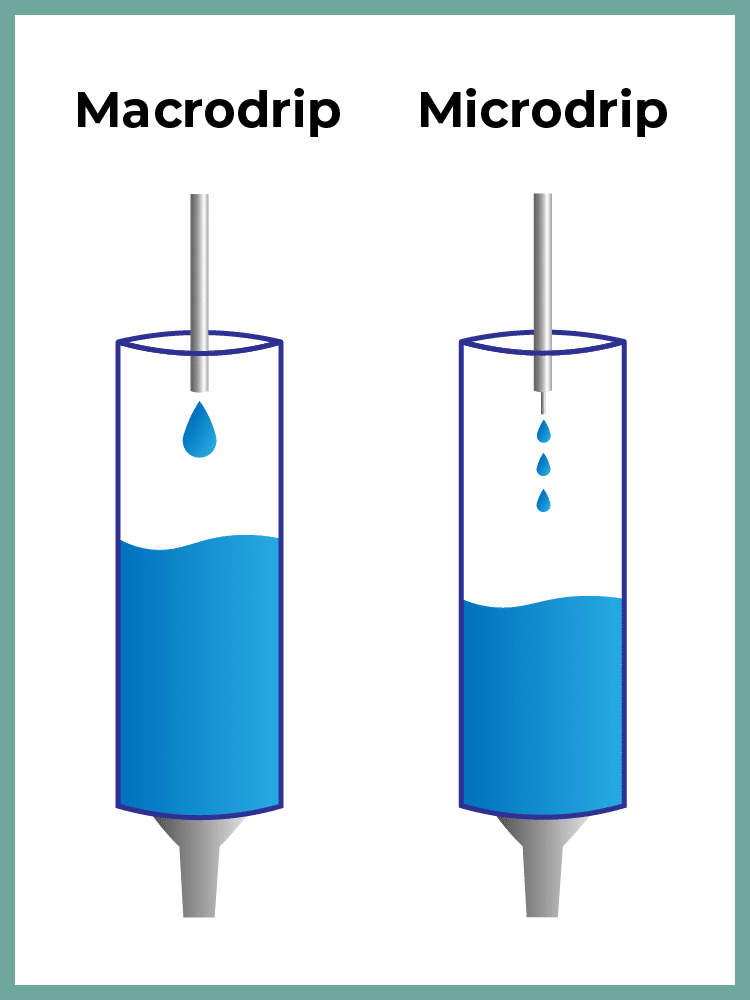
Microdrip Tubing
Microdrip tubing is used to produce small drip sizes. Typically used with potent medications or for populations with a narrow tolerance range (e.g. pediatric patients), microdrip tubing helps clinicians administer the appropriate amount of a medication without causing bloating or discomfort for the patient. The drip factor for a microdrip is typically estimated at 60 gtt/mL.
Macrodrip Tubing
Macrodrip is the more standard kind of IV tubing. It produces bigger drops to infuse larger amounts of fluid or infuse medications quicker. When using macrodrip tubing, it is important to monitor the patient for dehydration as the drop rate and fluid intake may be too low. This kind of tubing is typically available at 10, 15, or 20 gtt/mL.
Infusion Rate
The infusion rate is the volume of liquid that will be infused over a certain amount of time. To calculate this, you will need to know the total volume that you will be infusing and the total time that the infusion will take place. Depending on the units of measurement provided, you may need to convert your calculation to milliliters per hour.
Infusion Rate Formula:
Infusion Rate = volume to infuse in mL / time of the infusion in hrs
Example: You have 50 mL of a solution to infuse over 30 minutes.
Infusion Rate = (50 mL / 30 min) x (60 min/hr)
Infusion Rate = 100 mL/hr
IV Drip Rate
The IV drip rate is the measurement of the drops that fall into the drip chamber in a minute. It can be used to calculate the volume of liquid or medication a patient will receive in a certain amount of time.
The drip rate is determined using the drop factor of the tubing, the total volume needing to be infused, and the total time for the infusion. It is important to remember to round to the nearest whole number at the end of your calculations, as you cannot administer part of a drop.
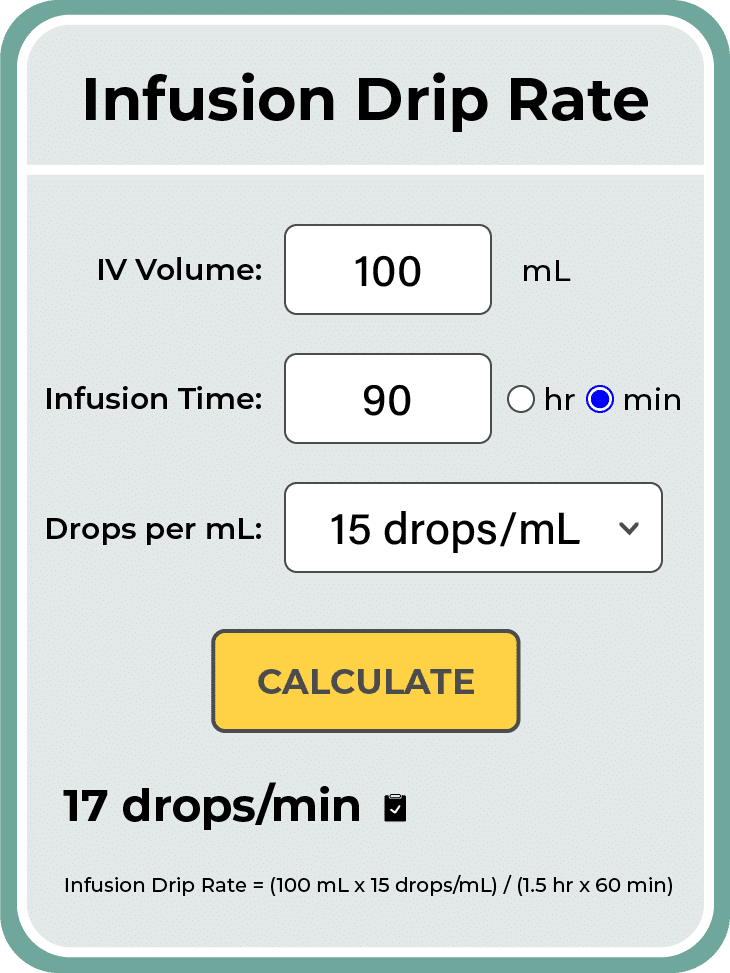
IV Drip Rate Formula:
Drip Rate = (volume to infuse in mL / time of infusion in min) x drop factor
Example: You have 100 mL of a solution to infuse over 90 minutes. The predetermined drop factor of the macrodrip tubing you are using is 15 gtt/mL.
Drip Rate = (100 mL / 90 min) x 15 gtt/mL
Drip Rate = 1500 gtt / 90 min
Drip Rate = 16.66 gtt/min = 17 gtt/min
There is also a simplified formula for calculating the IV drip rate that requires the infusion rate and simple division depending on the drop rate. For this method, you divide the infusion rate (mL/hr) by a predetermined number associated with the drop factor of the tubing.
Microdrip:
60 gtt/mL → divide by 60
Macrodrip:
10 gtt/mL → divide by 6
15 gtt/mL → divide by 4
20 gtt/mL → divide by 3
Example: Using the same example from above, you have 100 mL of a solution to infuse over 90 minutes. The predetermined drop factor of the macrodrip tubing you are using is 15 gtt/mL.
Drip Rate = ((100 mL / 90 min) x (60 min/hr)) / 4
Drip Rate = (100 x 60) / (90 x 4)
Drip Rate = 16.66 = 17 gtt/min
Infusion Conversions
As mentioned above, there are a few common conversions involved in infusion therapy that clinicians may find beneficial to memorize, but there may be instances when a conversion needs to be manually calculated. To do this, determine the unit that is currently being measured, the drug concentration, and the desired unit. For example:
To find mcg/min when given the infusion rate (mL/hr) and the drug concentration (mg/mL):
mcg/min = (mg/mL) x (1000 mcg/1 mg) x (mL/hr) x (1 hr/60 min)
Example: A patient is being infused with 50 mg/500 mL NaCL solution at a rate of 8 mL/hr. What dose (mcg/min) is the patient receiving?
mcg/min = (50 mg/500 mL) x (1000 mcg/mg) x (8 mL/hr) x (1 hr/60 min)
mcg/min = 400000 mcg / 30000 min = 13.3 mcg/min
To find mcg/kg/min when given the infusion rate (mL/hr), the drug concentration (mg/mL), and the patient weight (lbs):
mcg/kg/min = [(mg/mL) x (1000 mcg/1 mg) x (mL/hr) x (1 hr/60 min)] / (lbs) x (1 kg/2.2 lbs)
Example: A patient is being infused with 800 mg / 250 mL D5W solution at a rate of 16 mL/hr. The patient weighs 188 lbs. Calculate the weight-based rate.
mcg/kg/min = ((800 mg / 250 mL) x (1000 mcg/mg) x (16 mL/hr) x (hr/60 min)) / (188 lbs x (454 g/lb) x (kg/1000 g))
mcg/kg/min = (12800000 mcg / 15000 min) / (85352 / 1000 kg)
mcg/kg/min = (12800000 mcg / 15000 min) x (1000 / 85352 kg)
mcg/kg/min = 9.99 mcg/kg/min = 10 mcg/kg/min
Universal Formula
The universal formula, or the desired over have method, is a comprehensive formula that uses the following components to calculate the dose: the medication dosage prescribed (the desired amount: D), the dose on the medication container (the amount on hand: H), and the form and amount of the medication supplied (the volume: V).
Formula:
Dose = (desired amount / amount on hand) x volume OR dose = (D/H)V
Example: You need to administer 75 mg of a medication. The drug concentration available from the pharmacy is 15 mg/mL. How many mL will you need to administer a 75 mg dose?
Dose = (75 mg / 15 mg) x 1 mL
Dose = 5 mL
Dimensional Analysis (DA), or the Factor Label Method
Lastly, the dimensional analysis method, or factor label method, uses the conversion factors between systems of measurement that we’ve been using, but does not require memorizing specific formulas. Because of its formula flexibility, this method can be used for all dosage calculations.
There are four steps to using dimensional analysis:
- Determine the unit of measure needed and place this label in the left side of the equation.
- Place the information with the same unit of measure as the preceding denominator in the numerator on the right side of the equation (canceling out unwanted labels).
- Repeat step two until all unwanted labels have been eliminated.
- Solve to determine the correctly labeled answer. Do not round until you have the final answer.
Example: A patient is being infused with 30 mg/250 mL NaCL solution at a rate of 8 mL/hr. What dose (mcg/min) is the patient receiving?
mcg/min =
mcg/min = (30 mg / 250 mL) x (1000 mcg/mg)
mcg/min = (30 mg / 250 mL) x (1000 mcg/mg) x (8 mL/hr)
mcg/min = (30 mg / 250 mL) x (1000 mcg/mg) x (8 mL/hr) x (1 hr / 60 min)
mcg/min = (30 x 1000 x 8) mcg / (250 x 60) min
mcg/min = 16 mcg/min
OR
mcg/min =
mcg/min = (30 mg / 250 mL) x (1000 mcg/mg)
mcg/min = (30,000 mcg / 250 mL)
mcg/min = 120 mcg/mL
mcg/min = (120 mcg/mL) x (8 mL/hr) = 960 mcg/hr
mcg/min = (960 mcg/hr) x (1 hr / 60 min)
mcg/min = 960 mcg / 60 min
mcg/min = 16 mcg/min
The Importance of Appropriate Calculations
While there are many more abbreviations and IV calculations needed in the field of infusion, some being medication-specific, these are a few of the most commonly used formulas by clinicians.
According to a study conducted by the National Center for Biotechnology Information, miscalculations are one of the leading contributors to medication errors in intravenous and subcutaneous medication administration for in-hospital treatment.
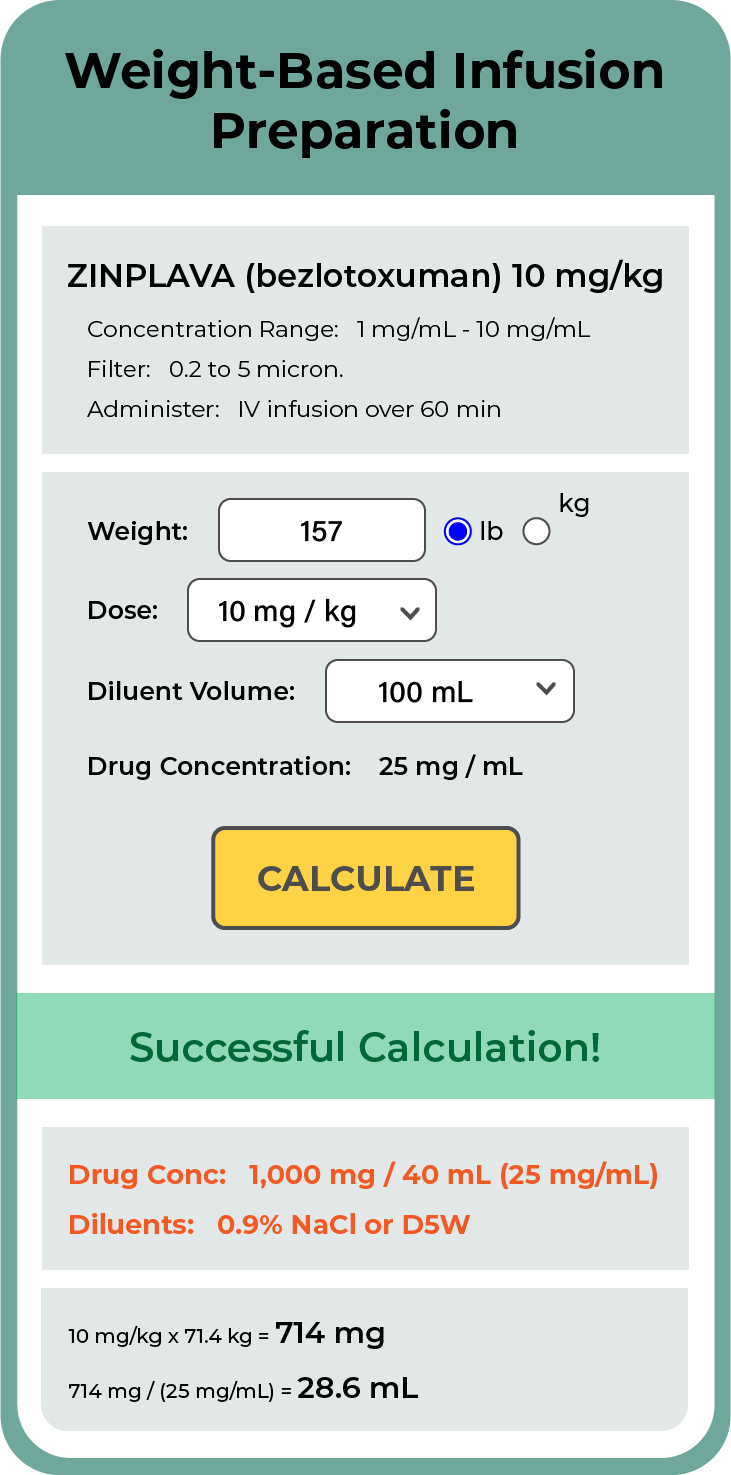
To eliminate some of the human error involved in miscalculations, RxToolKit has created pharmacist-approved quick calculators that allow users to input the relevant information and instantly receive accurate computations.
To enhance clinical competency, these calculators also provide the mathematical steps to reach the desired IV calculation, so clinicians can check their work or familiarize themselves with the manual processes to improve their understanding.
RxToolKit’s calculators can be found at the top of each medication monograph, or RxWorkFlow, and medication-specific checks and computations can be made throughout the preparation and administration process. This ensures that clinicians are not only accurate in their IV calculations and dosage conversions, but are using the correct formula for the specific step in the infusion process.
With confident clinicians, correct calculations, and comprehension of the common dosage conversions and infusion computations, we can minimize preventable medication errors and improve patient safety in our industry.
References:
BC Emergency Health Services. (n.d.). Infusion Drip Rate Formula. BCEHS. Visit resource.
Lin, A. (2022, January 6). Key factors influencing IV flow rate. KMED. Visit resource.
Mometrix Test Preparation. (2023, November 21). IV drip rate calculation formula – nursing review (video). Mometrix. Visit resource.
Pharmacy Calculations for Pharmacy Technicians: Concentrations, Dilutions and Drug Dosing. PowerPak. (n.d.). Visit resource.
Schnur, M. B. (2021a, July 23). Drug calculations: How to use the universal formula. NursingCenter. Visit resource.
Schnur, M. B. (2021b, August 16). Drug calculations: How to use dimensional analysis. NursingCenter. Visit resource.
Schnur, M. B. (2021c, December 6). Drug calculations: How to calculate drops per minute. NursingCenter. Visit resource.
Simple Nursing Editorial Team. (2018, December 3). Dosage calculations: IV drip factor formula. Simple Nursing. Visit resource.
University of Southern Queensland. (2018). Intravenous Infusion Calculations.
Wolters Kluwer. (n.d.). Drug calculations. NursingCenter. Visit resource.




