There’s been a shift in the registered nurse workforce signifying movement from hospital to ambulatory settings. We explore the challenges facing nurses, the differences in hospital vs. ambulatory settings, and what’s so intriguing about ambulatory care. We also interviewed Anand Patel, CEO of Infuse One, to share the perspective of an employer who often hires registered nurses from the hospital setting for his ambulatory organization.
Over the last six years, there has been an increase of approximately 400,000 registered nursing jobs in the United States and significant shifts in workplace demographics signifying RN movement from traditional hospital settings to ambulatory care.
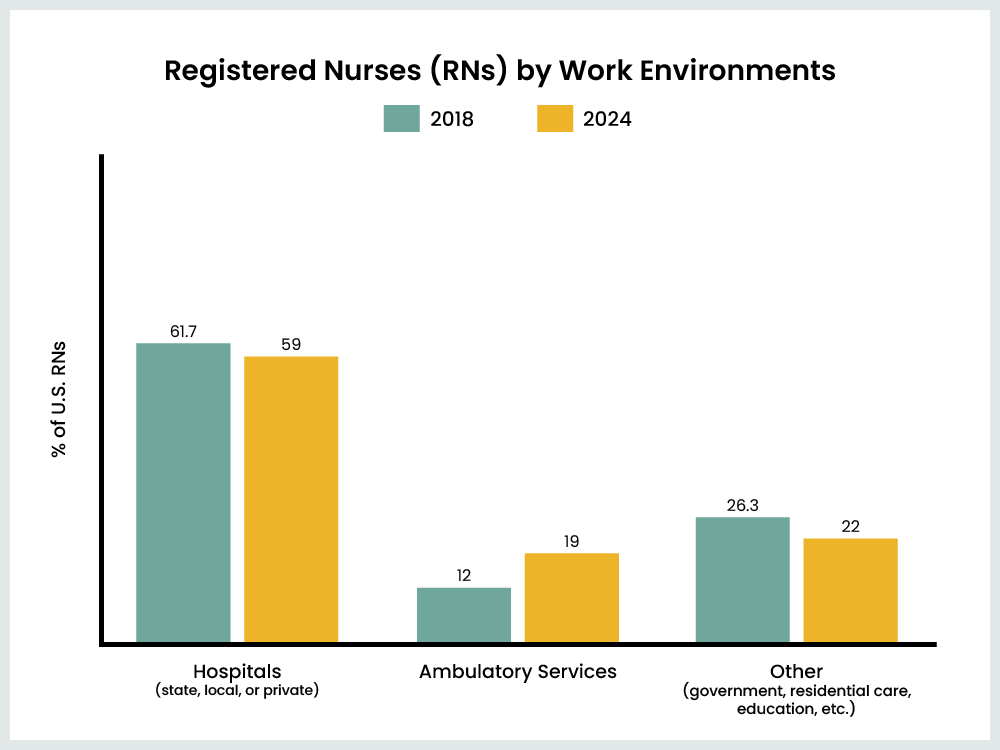
While hospitals continue to be the most prominent employer of registered nurses, ambulatory healthcare services, such as home healthcare and outpatient care, are becoming more popular.
In 2018, there were ~3.0 million registered nurses in the U.S., with 61.7% in the hospital setting, 12% in ambulatory services, and 26.3% in other inpatient and healthcare settings. In 2024, there were ~3.4 million registered nurse jobs, a 400,000 increase. 59% of those jobs were in hospitals, 19% were in ambulatory healthcare services, and the other 22% were in residential care facilities, government positions (excluding education and hospitals), and educational services.
The reason for this shift: nurse burnout, understaffing, education requirements and preferences, and the allure of ambulatory specialties.
What challenges are registered nurses facing?
The Nursing Shortage
Despite nursing being the nation’s largest healthcare profession, the U.S. is currently facing a workforce shortage. According to the U.S. Bureau of Labor Statistics (BLS), registered nurse employment is expected to increase 5% from 2024 to 2034, with approximately 189,000 openings each year. This growth will impact a variety of healthcare settings, such as hospitals and ambulatory care.
The growing demand for nurses is tied to the increasing elderly population (Americans over the age of 65), which is predicted to increase from 58 million in 2022 to 82 million by 2050; the prevalence of chronic conditions, which impacts 76.4% of U.S. adults; and in response to nurses either leaving the field for other occupations or retiring.
Staffing Struggles
Nurses frequently cite staffing levels as a main point of concern impacting their workload and employment. 68% rate “more nurses per patient” as “extremely important”, as it directly contributes to the quality of care patients receive and the stress levels of the registered nurse. This exemplifies the damage of the nursing shortage on the current workforce, and reinforces the need for more registered nurses in the field.
However, over one million nurses are predicted to retire from 2017 to 2030. The wave of baby-boomer nurses (nearly 660,000 in 2020) is expected to grow, with The U.S. Bureau of the Census Current Population Survey predicting nearly 80,000 annual retirements from registered nurses in the baby-boomer generation by the end of the decade.
But retiring isn’t the only way nurses are leaving the profession.
In AMN Healthcare’s 2024 Nurse Pulse Survey, 35% of nurses said it was “very likely” they would change jobs in 2024, and 58% said it was either “very likely” or “somewhat likely”. While the 2025 NSI National Health Care Retention & RN Staffing Report estimated only 16% turnover in 2024, the staggering statistics showcase nurse dissatisfaction and indicate a potential crisis for the healthcare industry.
COVID-19 Pandemic & Burnout
Prior to the COVID-19 pandemic, registered nurses had already been experiencing strain from the nursing shortage, which contributed to burnout, understaffing, and difficult schedules and hours. When COVID began, the demand for experienced nurses surged even higher to accommodate the patient numbers, and preexisting flaws in the healthcare system became more visible.
Approximately 5% of the nursing workforce (195,000 nurses) left the profession due to the pandemic, citing high-risk working conditions, burnout, inadequate staffing, and unsatisfactory safety protocols as contributing factors.
In acute care settings, burnout levels are particularly high, especially post-COVID. In national surveys following the pandemic, it was found that 60% of acute care nurses reported feeling burnt out; 75% reported feeling stressed, frustrated, and exhausted; and 66% considered leaving their profession after their experiences during the pandemic.
“The hospital environment just burns people out and they’re just looking to change their pace and their workflow and get a bit more family balance,” said Anand Patel, CEO of Infuse One, a multi-site ambulatory infusion organization. “They want to do something different. They want to cut the pace.”
Schedules & Working Hours
According to the 2024 Nurse Pulse Survey, 58% of nurses reported that “better schedules/hours” was “extremely important” to them, highlighting the value of time management and flexibility. Approximately 55% of surveyed nurses reported that they are either “extremely likely” or “somewhat likely” to change their hours or schedules within the current year.
For many nurses in hospital or acute care settings, shifts can last up to 12 hours and be scheduled for consecutive days. With the combination of burnout and understaffing, it’s clear that many registered nurses are dissatisfied with their work-life balance and value schedule flexibility as an essential factor contributing to their retention.
Pay
Among registered nurses’ desire for better hours and increased support, pay has also been a top priority impacting nurse satisfaction, with 75% rating “better pay rates for nurses” as “extremely important”. While many healthcare facilities have adjusted their compensation rates for registered nurses, pay remains a matter of key importance.
Education Requirements
Nurses are also experiencing a shift in educational requirements and preferences set forth by employers. As of 2022, the majority of nurses (72%) enter the field with a bachelor’s degree or higher, matching the 72% of healthcare employers with a strong preference for baccalaureate-educated nurses.
Unfortunately, the supply of highly educated nurses is struggling to meet the demand. Despite enrollment in entry-level nursing programs increasing by 0.3% in 2023, the American Association of Colleges of Nursing (AACN) reported a 3.1% and 0.9% drop in doctorate- and masters-level nursing programs, respectively.
According to the AACN report, nursing schools across the country turned down 65,766 qualified applications for undergraduate and graduate programs in 2023 due to insufficient faculty, clinical sites, classroom space, clinical preceptors, and budget constraints. In a Special Survey on Vacant Faculty Positions, nearly 80% of the vacant faculty positions were requiring or preferring a doctorate degree.
With masters- and doctorate-level enrollment in nursing programs dropping and the strong preference/requirements for these degrees in higher education faculty positions, there is a shortage of nurses with the necessary experience and education to help train the next generation of nurses that require said experience. This leads to the rejection of accepted applicants, impacting the number of nurses entering the field and further impacting the nursing shortage, staffing complications, and burnout nurses face.
While not a substitution for a formal educational degree, Infuse One utilizes clinical training and medication resource tools like RxToolKit to help make their nurses more comfortable with the medications they’re administering, and keep them updated on any changes to the drug guidelines.
“It’s a big change of environment and RxToolKit makes the drug part very easy for us because, you know, usually we train for a week at least, or maybe a little bit longer. But we give them access to RxToolKit…and we expect them to go through every single course on there specific to certain drugs that we regularly infuse,” said Patel. “It’s a game changer because I can’t call in a manufacturer’s rep every time I employ a new nurse. So this is a really good tool for just knowing that it’s done right, knowing that they’ve read something. They know where the package insert is. They know what the drug does. They know what it’s all about. They know how to infuse it. It’s kind of a peace of mind that it’s all in one place.”
What’s the difference between the hospital and ambulatory settings?
It’s undeniable that registered nurses have vital jobs, regardless of the setting they work in. From acute care to home healthcare, nurses consistently provide life-saving and -changing treatment for individuals of all ages, health conditions, and backgrounds.
To understand why registered nurses are shifting from hospitals to ambulatory settings, it’s important to understand the differences in their responsibilities, schedules, and long-term health effects.
What is the hospital setting?

Hospitals are community facilities that can offer care including intensive (emergency, serious illness, or injury), and nonintensive (childbirth, surgery, or recovery) care. These can include but are not limited to:
- Community, district, or federal hospitals
- General services hospitals
- Psychiatric hospitals
- Research hospitals
- Teaching hospitals
- Specialty hospitals
Responsibilities
Many hospital nurses treat patients with acute and even life-threatening conditions, and focus on emergency services that require consistent monitoring. They must be prepared for a variety of situations and medical emergencies, and their responsibilities can include:
- Taking vitals and noting symptoms
- Patient health assessments
- Updating records and documentation
- Collecting samples
- Educating patients about their condition and treatment
The hospital environment may expose nurses to greater infectious diseases, hazardous drugs, and radiation, requiring them to follow strict protocols for interacting with medications and equipment. Nurses are also expected to be able to spend hours on their feet standing, walking, or bending over to help move patients.
Due to the variety of conditions and treatments nurses experience in the hospital settings, they have many transferable skills that are valuable to other settings and specialties, such as infusion.
“What we do find is most nurses that have emergency room experience, especially in a hospital setting, do have really good vein access practices, where some nurses that may be working in a different environment, like an office of some kind, may not really have the practical experience of vein access,” said Patel.
Schedules & Pay
It is common for hospital nurses to work long, inconsistent shifts or even be on call. A registered nurse working three 12-hour shifts a week ranging between day, night, and weekend, is typical. This schedule may allow nurses to have multiple days off per week, but requires extreme flexibility for varying shift assignments week to week.
Nursing salaries vary depending on the organization, state, and department, but according to the BLS, the median annual wages for registered nurses working in hospitals was $97,260 in 2024, only topped by the wages for government (excluding education and hospitals) nurses at $106,480. The BLS reported that hospital nurses commonly experience more opportunities for career advancement and mobility, and therefore earn higher wages.
What is the ambulatory setting?
The ambulatory setting encompasses locations providing care on an outpatient basis, particularly those focused on preventative care or treatment of chronic conditions, such as:
- Retail clinics
- Physician offices
- Home healthcare
- Urgent care centers
- Specialty care centers
Responsibilities
Because ambulatory nurses often specialize in certain areas, such as women’s health or pediatrics, their responsibilities heavily depend on the specific provider setting they work in, but can include:
- Gathering and documenting patient medical history, concerns, and symptoms
- Working with doctors and other clinicians to assess the patient’s condition
- Preparing and/or administering treatment or medication
- Maintaining medical equipment
- Educating patients about their condition and treatment
- Establishing a maintaining relationships with returning patients
As ambulatory settings are more likely to have repeat patients who live with chronic diseases or have frequent checkups, nurses have the opportunity to build short- or long-term relationships with patients and their families.
“I think the big thing is nurses like the work pattern, meaning it’s more of a relaxed job than in an emergency room or a hospital or any other setting. It’s fulfilling,” said Patel. “We’ve had nurses that just started with and worked only one day a week or twice a week maybe, and they’ll come back and say, I really like this. They get to build longstanding bonds with the patients because, basically, chronic disease patients come for a long period of time and they keep on coming back.”
Schedules & Pay
Unlike hospital registered nurses, ambulatory nurses are more likely to work a 9-to-5, Monday-through-Friday schedule. This means they have a traditional two-day weekend, but have a more predictable schedule to help maintain work-life balance and routines.
“As an infusion center, we can offer them 9-to-5 kind of hours, but more socially-based for their environment, I suppose. We can offer them a great rate of pay and we can train them very easily with RxToolKit on the medications. So we found it’s been a good fit for us and for the nurses,” said Patel.
According to the BLS, average median wages for registered nurses in ambulatory healthcare services was $83,780 in 2024, fitting between hospital nurses at $97,260 and nursing and residential care facilities nurses at $81,820.
The Future for Hospitals & Ambulatory Care
It isn’t just the workforce shift that’s affecting this change, but the economics and expectations of healthcare. Due to the increasing pressure from payors to reduce the cost burden on the healthcare system, high-cost hospital therapy is anticipated to shift to lower-cost ambulatory sites, like infusion centers or patient homes.
In the ambulatory infusion market alone, the aging population and rise in chronic conditions has increased demand for therapy. According to the National Infusion Center Association (NICA), the infusion therapy market has an expected 8.9% Compound Annual Growth Rate (CAGR) projection through 2030.

The cost of a single infusion treatment varies drastically depending on the site of care, with hospitals costing an average of $5,500 to $11,500 per infusion, ambulatory infusion centers $3,500 to $5,000, and home infusion therapy $1,700 to $3,500.
AICs are often overseen and staffed by a team of registered nurses specializing in infusion therapy, and nurses working in the home infusion industry travel to the patient’s home to administer treatment. While hospitals were the first site of care to offer infusion therapy and remain the primary setting, this is expected to decline in the next few decades as alternative lower-cost options gain popularity.
What’s so great about working in the ambulatory setting?
 The migration of registered nurses from hospitals to ambulatory settings is only one sign of the growing popularity of ambulatory healthcare settings. Between burnout, nurse shortages, inconsistent schedules, and the difference in relationships with patients, nurses are seeking out alternative environments (like Infuse One) to grow their careers.
The migration of registered nurses from hospitals to ambulatory settings is only one sign of the growing popularity of ambulatory healthcare settings. Between burnout, nurse shortages, inconsistent schedules, and the difference in relationships with patients, nurses are seeking out alternative environments (like Infuse One) to grow their careers.
With more predictable hours, more consistent staffing, the opportunity to build lasting relationships with patients, and the predicted industry growth over the next few decades, transitioning into the ambulatory setting is looking like a strategic option for registered nurses.